An ostomy, or stoma, is a surgically created opening in the abdominal wall that allows the intestines to drain out the surface of the abdomen. A circular incision is made in the abdominal wall and a piece of intestine is brought through the incision to lie partially outside the body wall. The part of the bowel that is seen on the abdomen surface is called a stoma. Ostomies are often created as a part of intestinal surgery when there must be a new way for intestinal waste to leave the body. The most common types of ostomy connect either the small intestines (ileostomy or jejunostomy) or the large intestine (colostomy) to the abdominal wall. Ostomies can be temporary or permanent. This information was prepared to help patients understand what an ostomy is, learn how to live with an ostomy, relieve concerns they may have and assure them that they can enjoy an active and fulfilling life with an ostomy.
REASONS FOR AN OSTOMY
- Cancer
- Trauma
- Inflammatory bowel disease (IBD) such as Crohn’s disease or ulcerative colitis.
- Bowel obstruction
- Infection
- Fecal incontinence (inability to control bowel movements)
- Constipation
- Diverticular disease (small bulges or sacs that form in the wall of the large intestine)
OSTOMY TYPES
Your surgeon can answer questions about the type of ostomy you have:
-
Ileostomy: Connects the last portion of the small intestines (ileum) to the abdominal wall.
-
Colostomy: Connects a portion of the colon (large intestine) to the abdominal wall.
-
Temporary ostomy: This is an ostomy that can be removed surgically at a later time. It is generally made from the small intestines (ileostomy). It prevents the passage of stool through the intestines below the stoma. Often a temporary ostomy is created to allow the intestines to heal after surgery or from a disease such as diverticular disease or Crohn’s disease.
-
Permanent ostomy: This ostomy is created when there is not an intention to reconnect the bowel. This is an ostomy that is used when parts of the rectum, anus and colon have been removed due to disease or treatment of a disease. It may also be done when the muscles that control elimination are removed or are no longer functioning properly.
-
End ostomy: This ostomy has one end of a segment of bowel come through the skin opening.
-
Loop ostomy: This ostomy can also be called a diverting ostomy and is typically formed when there is a plan to reconnect the bowel at a later time. Two ends of the bowel come through the skin opening and you may see two openings of the bowel. A loop ostomy may appear larger than an end ostomy because of the two openings. This may make fitting an appropriate appliance for a loop ostomy slightly more challenging.
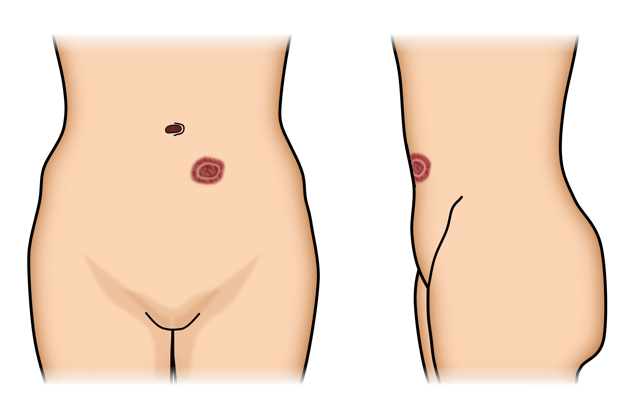
Figure 1: An ostomy connects either the small or the large intestine to the abdominal wall.
THE OSTOMY BAG
After an ostomy is created, bowel movements occur through the opening in the abdominal wall or stoma. An ostomy appliance is a bag that catches and holds the stool. The ostomy appliance consists of a wafer and plastic bag. The wafer sticks to the abdominal wall with adhesive. The bag is disposable and emptied or replaced as needed. This system is secure, odor-free and accidents are uncommon.
OSTOMY PLACEMENT
Prior to surgery, your surgeon or Wound, Ostomy and Continence (WOC) nurse will examine your abdomen to find a suitable place on your abdominal wall for the opening or stoma. An ostomy is best placed on a flat portion of the front of your abdomen that is easy to see. A colostomy is usually placed to the left of the navel and an ileostomy to the right.
A wound ostomy continence nurse (WOC nurse or enterostomal therapist) is a registered nurse who has additional education and training on how to care for patients who have an ostomy, and may assist your colorectal surgeon in helping you plan, care for and live with your ostomy.
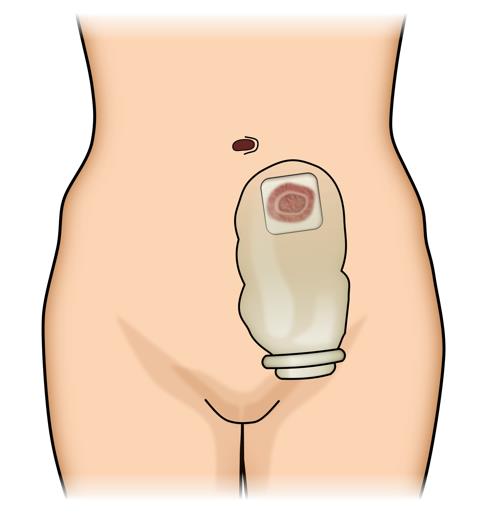
Figure 2: An ostomy appliance is a plastic pouch. It is held to the body with an adhesive skin barrier that provides secure and odor-free control of bowel movements.
POSTSURGICAL CARE
You will be taught how to use the ostomy bag by a WOC nurse or enterostomal therapist and your colon and rectal team. The doctors, advanced practitioners, and nurses will work with you on any necessary changes to your diet.
Early after surgery, the stool from an ileostomy is generally a liquid type of drainage. However, as the small intestine begins to adapt, the stool will become thicker and more paste-like. Stool from a colostomy is generally pasty and semi-formed.
The frequency and volume of bowel movements vary from person to person. Your bowel movements will depend on how often you went to the bathroom prior to surgery, the type of ostomy that was placed, the type of surgery that was done and your dietary habits.
With an ostomy, you can shower or bathe just as you did before. Soap and water will not flow into your stoma or hurt it in any way. You may shower or bathe with your pouch on or off – the choice is yours.
You may need to empty your ostomy bag several times per day but will likely only need to completely remove the ostomy appliance from your skin two to three times per week.
DIETARY RESTRICTIONS
Depending on the type of ostomy, you may need to change what you eat and when you eat to control the number of and consistency of bowel movements. You will learn to monitor the effect of food on ostomy function. After a period of time, many patients are able to slowly introduce foods back into their diets. It helps to chew food well, drink plenty of fluids and avoid certain high roughage foods, such as green leafy vegetables. After recovering from surgery, most patients do not have dietary limitations.
You will learn to monitor the amount and consistency of your bowel movements. The average daily output of an ileostomy is about 500 mL per day but may be up to 1,000-1,500mL in a day. The average daily output of a colostomy is about 500mL per day, with a range of about 200-700mL. Outputs consistently above average levels may put patients at risk for dehydration. Very low or no output from the ostomy is concerning for obstruction or blockage. Contact your surgical team if you have very high watery output or no output at all.
PHYSICAL RESTRICTIONS
All activities including recreational sports, exercise, swimming and travel may be resumed once healing from surgery is complete. There are many variations of ostomy appliances adapted to certain activities. Your WOC nurse can help teach you about options for different activities and give you practical tips. Public figures, famous entertainers and even professional athletes have ostomies that do not limit their activities.
Most patients with ostomies are able to resume their usual sexual activity. Some patients worry that their sexual partner will not find them attractive due to the ostomy bag. This change in body image can be overcome. A strong relationship, time, patience and support groups all help address these problems.
WILL PEOPLE KNOW I HAVE AN OSTOMY?
Unless you tell someone, they won’t know that you have an ostomy. An ostomy is easily hidden by most clothing. You have probably met people with an ostomy and did not realize it. Some patients find that explaining the ostomy to people closest to them is a healthy way to cope with emotions.
While many patients worry that the pouch will be visible under their clothing, an ostomy is easily hidden by usual clothing. The ostomy appliance pouches are low profile and fit close to the body. The pouch can be worn inside or outside your underwear, whichever is more comfortable.
POST-OSTOMY PROGNOSIS
An ostomy can have complications. In the beginning, it may take some time to adjust to the way the appliance fits and empties. During this time, accidents, or leakage from the bag, may happen. Once you are used to the stoma wafer and bag, most common problems, such as local skin irritation, are easily treated. Major changes in weight loss or gain can affect how the ostomy sits on your abdomen. Some people develop a hernia (weakening of the abdominal wall around the ostomy) or prolapse (a protrusion of the bowel). These problems require surgery only if they cause major symptoms.
Dehydration may occur if there is loose watery stool output that is high in volume. Signs of dehydration can be subtle and range from dry mouth, reduced and dark urine, nausea, weakness, muscle cramps and feeling weak. You should replenish your body by drinking plenty of fluids, including some sports drinks with balanced electrolytes. With severe dehydration, patients may need to be hospitalized and given intravenous fluids.
Intestinal obstruction or bowel blockage can occur after any abdominal surgery. Signs of blockage may include abdominal pain, cramps, sudden decrease in output, or clear watery output. Food blockage can occur when high fiber foods that had been poorly chewed or digested form a clump that causes blockage. While most often obstruction resolves with supportive care and bowel rest, it is important that you contact your colorectal surgeon and your WOC nurse if you have these symptoms.
Living with an ostomy requires a period of learning and adjustment, but you can expect to enjoy a healthy and fulfilling life with your ostomy. Your colon and rectal surgeon and WOC nurse will provide necessary assistance and support.
WHAT IS A COLON AND RECTAL SURGEON?
Colon and rectal surgeons are experts in the surgical and non-surgical treatment of diseases of the colon, rectum, and anus. They have completed advanced surgical training in the treatment of these diseases, as well as full general surgical training. Board-certified colon and rectal surgeons complete residencies in general surgery and colon and rectal surgery, and pass intensive examinations conducted by the American Board of Surgery and the American Board of Colon and Rectal Surgery. They are well versed in the treatment of both benign and malignant diseases of the colon, rectum and anus and are able to perform routine screening examinations and surgically treat conditions, if indicated to do so.
DISCLAIMER
The American Society of Colon and Rectal Surgeons is dedicated to ensuring high-quality patient care by advancing the science, prevention and management of disorders and diseases of the colon, rectum and anus. These brochures are inclusive but not prescriptive. Their purpose is to provide information on diseases and processes, rather than dictate a specific form of treatment. They are intended for the use of all practitioners, health care workers and patients who desire information about the management of the conditions addressed. It should be recognized that these brochures should not be deemed inclusive of all proper methods of care or exclusive of methods of care reasonably directed to obtain the same results. The ultimate judgment regarding the propriety of any specific procedure must be made by the physician in light of all the circumstances
presented by the individual patient.
Would you like additional information about ostomies?
www.ostomy.org – The United Ostomy Associations of America
www.wocn.org - The Wound, Ostomy, and Continence Nurses Society
Surgical Patient Education, Ostomy Home Skills, Program website: https://www.facs.org/education/patient-education/skills-programs/ostomy-program